Table of Contents
Lymph Node
The lymph node is a part of lymphoid organs and the body’s immune system is a complex, kidney-shaped structure usually
located at the junction of several lymph vessels. From an anatomic
perspective, nodes consist of a cortex (outer portion),
a paracortex, and a medulla (inner portion).
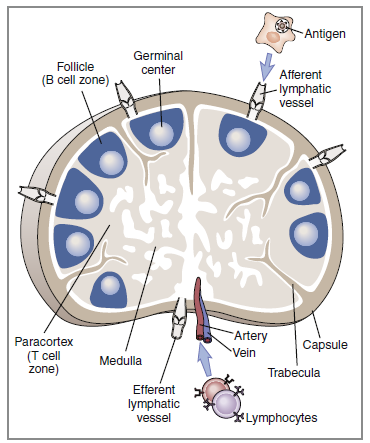
The cortex is densely packed with lymphocytes and
macrophages.
Primary follicles of virgin or naïve B cells, interspersed
in a framework of follicular dendritic cells, are prevalent in the outer cortex. When B cells are actively proliferating within
a follicle, the central area is referred to as the germinal center. Surrounding
the germinal center is the mantle layer that contains
B memory cells. Interspersed between the follicles is the paracortical
region. The paracortex contains CD4 helper cells, a few cytotoxic
CD8 cells, macrophages, granulocytes, and neutrophils.
The medulla, or the middle region of a lymph node, consists
of a series of cavernous, cellular cords and connecting
sinuses containing macrophages and plasma cells. Lymphoid
tissue containing B cells and histiocytes is arranged in medullary
cords between the connecting sinuses. Lymph fluid containing
T cells and plasma cells flows into medullary sinuses
and into efferent lymphatic vessels.
Spleen
The spleen, the largest lymphoid organ in the body, is located
in the upper left quadrant of the abdomen and tucked under
the diaphragm. The parenchyma or splenic bulk is divided
into red and white pulp.
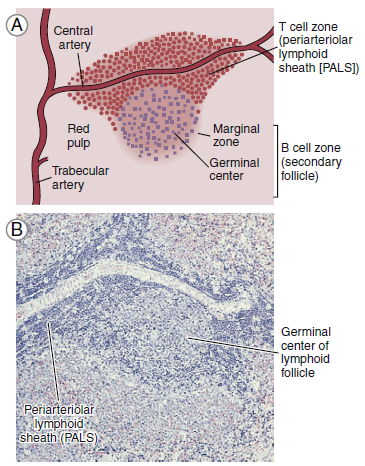
The red pulp contains splenic sinuses with numerous thin-walled
blood vessels interspersed between strands of connective
tissue. Sinuses filter foreign material and purify the blood. Old
or damaged red blood cells are concentrated and destroyed
by macrophages within venous sinuses. Sinuses also serve as storage facilities for platelets and red blood cells. Over 30% of platelets are sequestered in the spleen. On-demand, platelets
are expelled by the simple contraction of the organ.
White pulp is composed of lymphocytes that are clustered
around and along the length of small, central splenic arteries
to form a periarteriolar lymphoid sheath (PALS). Two-thirds of
the PALS are made up of CD4+ cells. B cells are also found in
the PALS in the form of primary follicles and germinal centers.
Along the rim of each splenic follicle is the marginal zone, which
contains a mixed population of virgin and memory B cells. Marginal zone B cells are unique in that they produce antibodies directed toward carbohydrate antigens.
Lymphoid tissue is organized into anatomic units
Mucosal-Associated Lymphoid Tissue
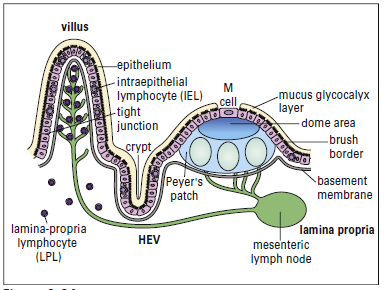
lymphoid tissue
Lymphocytes are scattered beneath the epithelium along the
entire gastrointestinal tract. Organized lymphocyte clusters,
called Peyer’s patches, are found in the ileum. Under light microscopy, Peyer’s patches appear as lymphoid follicles that contain CD4+ T helper cells, mature B cells, macrophages,
and dendritic cells. Surrounding the follicle is a mantle
of B cells that are analogous to the splenic marginal zone B cells.
Lymphocytes are found in the connective tissue and in the
epithelial layer of the mucosa. Intraepithelial Lymphocytes
(IELs) are found in the surface epithelium and have the closest
contact with bacteria and parasites. These lymphocytes
express CD8 and are constitutively cytotoxic. The exact function
of IELs is difficult to determine because both the phenotype
and the function differ depending on anatomic location.
Lamina propria lymphocytes (LPLs) are T cells and activated
B cells and plasma cells that produce specialized antibodies
are released into the intestinal lumen.
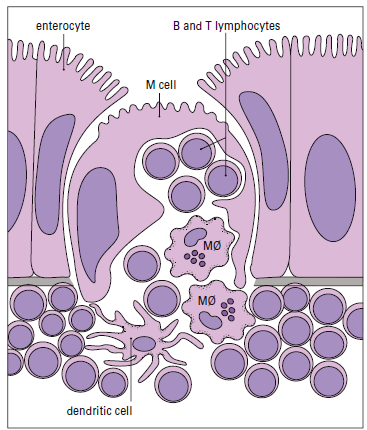
In the intestine, antigens are recognized by intestinal
microfold (M) cells present in the dome epithelium of Peyer’s
patches. These cells lack the villi normally present
on intestinal cells and have deeply invaginated basal surfaces
that trap antigens. Antigens are endocytosed by M cells,
transported in vesicles to the submucosa, and exocytosed to
lymphocytes in the intraepithelial spaces.
After antigenic stimulation in the intestinal mucosa, T cells
and antigen-presenting macrophages travel to the mesenteric
lymph node where the immune response is amplified. Lymphocytes
activated in the node enter the thoracic duct, which
empties into the bloodstream. After entering the
peripheral circulation, activated lymphocytes are evenly distributed
to mucosal tissues in the genitourinary tract, lung,
salivary and lacrimal glands, lactating mammary glands, and
the gut intestinal mucosa. Therefore, antigenic stimulation of
one mucosal surface provides protection to all mucosal surfaces.
After localization in mucosal tissue activated B cells initiate
the production of specialized secretory antibodies.
Tonsils
The entrance to the respiratory tract is guarded by tonsils,
which are localized in three areas of the oral pharynx. (1) Palatine
tonsils are found on the lateral wall of the oral pharynx.
They are covered with respiratory squamous epithelium and
surrounded by a capsule of connective tissue. (2) Lingual tonsils
are found at the root of the tongue. Both the palatine and
lingual tonsils have deep crypts that increase the surface area
available to trap bacteria and other antigens. (3) A third tonsillar
tissue is the pharyngeal tonsil or adenoid that is located in
the roof of the pharynx behind the soft palate.
Tonsils are lymphoid organs. All three tonsils are densely
packed with subepithelial and intraepithelial lymphocytes.
Subsets of CD4 and B cells, along with macrophages, are the
major constituents of tonsils. Tonsils produce secretory antibodies
aimed at diphtheria, Streptococcus, and a number of
respiratory viruses including polio and rubella viruses. The
removal of tonsils (tonsillectomy) severely reduces the production
of secretory antibodies and may increase the risk for
repeated infections of the oropharynx.